Courtney Sexton in Smithsonian:
 Humans are almost constantly connected to devices and electronics that generate a significant amount of data about who they are and what they do. Many commercially available products like Fitbits, Garmin trackers, Apple watches and other smartwatches are designed to help users take control of their health, and tailor activities to their lifestyle. Even something as unobtrusive to wear as a ring can collect data on sleep patterns, body temperature, heart rate variability, calorie burn, and steps, and even go a step beyond to analyze these biostatistics and package the information so it can be read on a user’s smartphone. Similar, less common but more precise monitoring devices are also being used at clinics and hospitals to help health care providers individualize treatments for a range of conditions from cardiac care to stroke rehabilitation. Researchers working to contain COVID-19 are increasingly turning to these sleek new wearables for a diagnostic solution. But there is some debate about the best way to do so. Can commercially available devices be leveraged as a tool, or would clinical-grade wearables be more effective?
Humans are almost constantly connected to devices and electronics that generate a significant amount of data about who they are and what they do. Many commercially available products like Fitbits, Garmin trackers, Apple watches and other smartwatches are designed to help users take control of their health, and tailor activities to their lifestyle. Even something as unobtrusive to wear as a ring can collect data on sleep patterns, body temperature, heart rate variability, calorie burn, and steps, and even go a step beyond to analyze these biostatistics and package the information so it can be read on a user’s smartphone. Similar, less common but more precise monitoring devices are also being used at clinics and hospitals to help health care providers individualize treatments for a range of conditions from cardiac care to stroke rehabilitation. Researchers working to contain COVID-19 are increasingly turning to these sleek new wearables for a diagnostic solution. But there is some debate about the best way to do so. Can commercially available devices be leveraged as a tool, or would clinical-grade wearables be more effective?
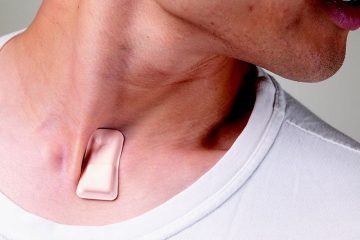
In April, the Journal of the American Medical Association identified fever, cough and shortness of breath as primary symptoms in both positive and false negative COVID-19 cases. Around the same time, medical thought leaders in the Chicago area approached John Rogers, the director of Northwestern University’s Querrey Simpson Institute for Bioelectronics. Rogers and his team are known for developing next-generation, flexible, wearable devices with clinical-grade monitoring capability that mount on relevant body areas. The patches look and feel much like a Band-Aid, but contain biosensors, onboard memory, data processing and wireless transmission features. The quality of data the devices can capture is high enough that they can reliably be used in settings and on patients with limited hospital access to run specialty-care tests like electrocardiograms (EKGs). Others reduce the need for complicated machines used to monitor premature infants in intensive care units.
More here.
